Digital Patient Education: Implementation guide for clinics
In many facilities in the DACH region, digital education is no longer an issue for the future, but a strategic necessity. Rising documentation requirements, increasing specialization, economic pressure and changes in patient information behavior are exacerbating the structural weaknesses of traditional information processes. At the same time, the legal and ethical responsibility remains high: effective consent requires that patients actually understand the nature, scope, risks, alternatives and consequences of a measure.
There is a gap between legal requirements, organizational reality and everyday clinical practice. Digital information promises efficiency, standardization and legal security. But its implementation is not an IT project. It is a far-reaching intervention in medical, legal and organizational processes. This guide shows what is strategically important – for hospitals as well as for doctors in private practice.
1. the structural problem of classical enlightenment processes
In practice, information is often provided under time pressure, depending on the situation and individual communication styles. Paper-based forms are completed, annotated by hand, signed and archived. In complex care settings – for example in anesthesia, orthopedics or interventional cardiology – content varies depending on the surgeon, resident or outpatient day.
The weaknesses of this system are structural:
- Content inhomogeneity: Even with identical interventions, formulations, risk presentations and priorities differ considerably.
- Documentation risk: Illegible additions, missing dates or incompletely completed forms can be problematic in the event of a dispute.
- Inefficiency: Repeated verbal explanations of standardized interventions tie up medical resources without proportionally increasing the gain in knowledge.
- Cognitive overload: Patients often receive complex information in an emotionally stressful situation – shortly before a procedure or as part of a tight practice schedule.
Digital education addresses these weaknesses – provided it is not misunderstood as the mere digitization of paper forms.
2. digital education is not a PDF on the tablet
A common misconception is to equate digitality with electronic signatures. However, a scanned form on a tablet does not change the quality of the content or the cognitive structure of the information.
Digital education only develops its added value when it:
- medical content in a structured, visually supported and comprehensible way,
- provides standardized, quality-assured content,
- individual risk constellations are taken into account in a differentiated manner,
- is integrated into existing systems in a documentation-safe manner,
- and complements the medical dialog, not replaces it.
The didactic and procedural architecture is crucial. Video-supported sequences can explain complex issues – such as surgical procedures, anesthesia procedures or typical complications – in a consistent and comprehensible way. However, generic videos quickly reach their limits: An elective arthroscopic procedure on an active 25-year-old is structurally different from a complex revision on a patient with multiple morbidities.
This reveals a key differentiating factor of modern systems: modular individualization.
3. modular individualization instead of one-size-fits-all
Many digital solutions work with standardized complete videos for each procedure. Although these are standardized, they are often too general or too extensive. The result: an unnecessary information burden or a lack of specificity.
A modular system, on the other hand, allows video sequences to be put together individually on the basis of defined criteria:
- Type and variant of intervention
- Anesthesia procedure
- Risk profile (e.g. anticoagulation, previous illnesses)
- Age group or special patient groups
- Special organizational features (e.g. outpatient vs. inpatient)
The structural advantages of this modular individualization are considerable:
- Cognitive efficiency: Patients only receive the content that is relevant to them – neither too much nor too little.
- Legal robustness: The documentation reflects exactly what content was taught.
- Role and specialist specificity: Different specialist departments can use specific modules without producing redundant content.
- Scalability: New procedures or guideline changes can be adapted at module level without having to produce complete new content.
Especially in the DACH context, where the requirements for informed consent are high and courts regularly examine whether risks have been explained in a sufficiently individualized manner, this differentiation is not a technical detail, but a strategic advantage.
4 Regulatory framework: What needs to be considered during implementation
Digital education is a field of tension between professional law, civil law, data protection and organizational responsibility. Even if a comprehensive legal assessment in individual cases is reserved for specialized lawyers, basic guidelines can be named.
In Germany, for example, the medical duty to inform is based on Section 630e BGB. The decisive factor is the provision of personal, timely and comprehensible information about the essential circumstances of the procedure. Digital elements can support this obligation, but cannot replace it. The medical consultation remains indispensable.
For implementation, this means
- Digital content must be embedded as preparatory and structuring elements in a face-to-face meeting.
- The time of provision must be sufficiently in advance of the procedure so that patients have time to think about it.
- The documentation must clearly show what content was taught and when.
- Data protection requirements (GDPR) must be taken into account, especially for cloud-based solutions.
For clinics, close coordination with the data protection officer, legal department and quality management is recommended. In private practices, a structured risk analysis should at least be carried out, especially when using external platforms.
5 Organizational implementation: from pilot project to routine
Technically, the introduction of digital education systems is usually faster than their cultural anchoring. Resistance arises less from rejection of digitality than from uncertainty regarding role changes.
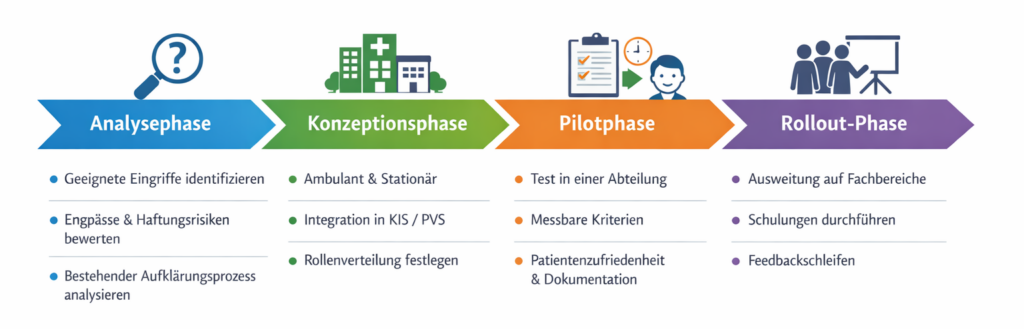
A structured implementation process typically comprises the following phases:
- Analysis phase:
Which interventions are suitable for initial implementation? Where are there currently bottlenecks or liability risks? How is the existing information process organized? - Concept phase:
Definition of the target architecture: outpatient/inpatient, pre-inpatient integration, integration into HIS/PVS, distribution of roles between doctors and nursing staff. - Pilot phase:
Start in a clearly defined department with measurable parameters: duration of the consultation, patient satisfaction, completeness of documentation. - Rollout phase:
Gradual expansion to other specialist areas, accompanied by training and feedback loops.
It is crucial to communicate digital education not as a tool to relieve the burden on individuals, but as a structural quality measure. It professionalizes processes – and makes them more transparent at the same time.
6. psychological dimension: control, trust and acceptance
Information is not only a legal obligation, but also a key act of trust. Digital formats can strengthen this trust – or undermine it.
Patients often appreciate being able to view content in a quiet environment with the option of repeating sequences. Visual representations of complex processes increase understanding. At the same time, the impression must not be created that the personal conversation is being “replaced by a video”.
There are also implicit fears on the part of doctors: Loss of individual creative freedom, standardization of communication or additional technical hurdles.
A clear positioning helps here: digital education structures the information space. The medical consultation remains the place for individual risk assessment, classification and answering personal questions. Standardization does not mean incapacitation, but quality consistency.
7. practical example: Pre-inpatient information in orthopaedics
An orthopaedic clinic with a high volume of knee arthroscopies was faced with the problem that explanatory discussions often took place the day before the operation. Time pressure, repeated standard explanations and incomplete documentation led to dissatisfaction on both sides.
With the introduction of a modular digital information system, patients were provided with individualized video sequences several days before the procedure – differentiated according to the type of procedure, anesthesia method and specific risk factors.
The content of the medical consultation shifted: less basic information, more focus on individual questions and special features. At the same time, it was possible to document which modules were viewed and when the personal interview took place.
The structural change was not primarily in the technology, but in the time equalization and in the clear distribution of roles between standardized information transfer and individual medical advice.
8 Strategic classification: Digital education as a building block of process quality
Digital education should not be viewed in isolation. It is part of a more comprehensive digital preclinical strategy: appointment management, medical history taking, document management and process control are all interlinked.
Their strategic value lies in three dimensions:
- Quality: Standardized, modular content increases consistency and traceability.
- Efficiency: doctors’ time is more focused on individual decision-making aspects.
- Legal protection: Transparent documentation strengthens the position in the event of liability, without replacing individual examination in each case.
Particularly in complex organizations with multiple locations, changing personnel and different specialist disciplines, modular, individualized digital education creates a common basis in terms of content – without losing the necessary differentiation.
Conclusion: From digitalization to structural redesign
The implementation of digital education is not a technical upgrade, but a structural redesign of medical communication processes. Those who reduce it to electronic signatures are wasting its potential. Those who see it as a strategic instrument for standardization, individualization and legal robustness, on the other hand, create a new level of quality in the preclinical workflow.
In an increasingly specialized, liability-sensitive and resource-limited healthcare landscape in the DACH region, digital education is thus becoming a crucial component of professional organizational development. Not as a replacement for medical responsibility – but as systematic, scalable and differentiated support for it.